What is the temporomandibular joint (TMJ)?
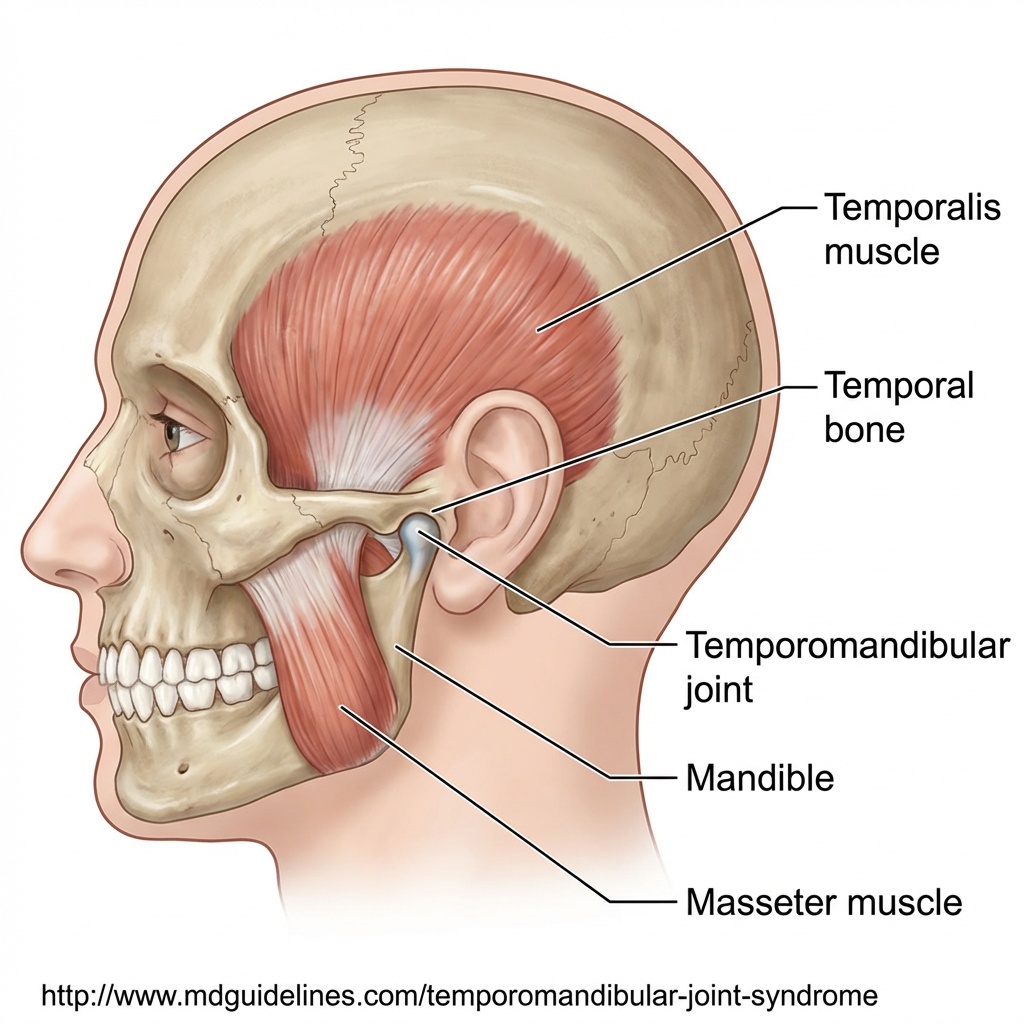
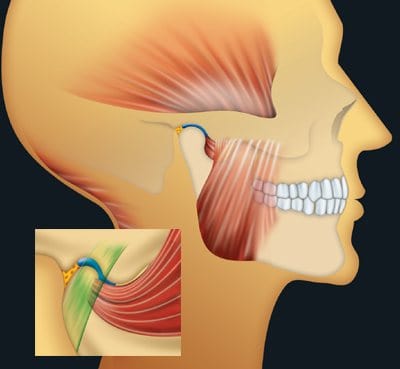
The temporomandibular joint (TMJ) is the joint that connects your lower jaw (mandible) to the temporal bones of your skull, on each side of your face, just in front of the ears. It is one of the most complex and most used joints in the human body.
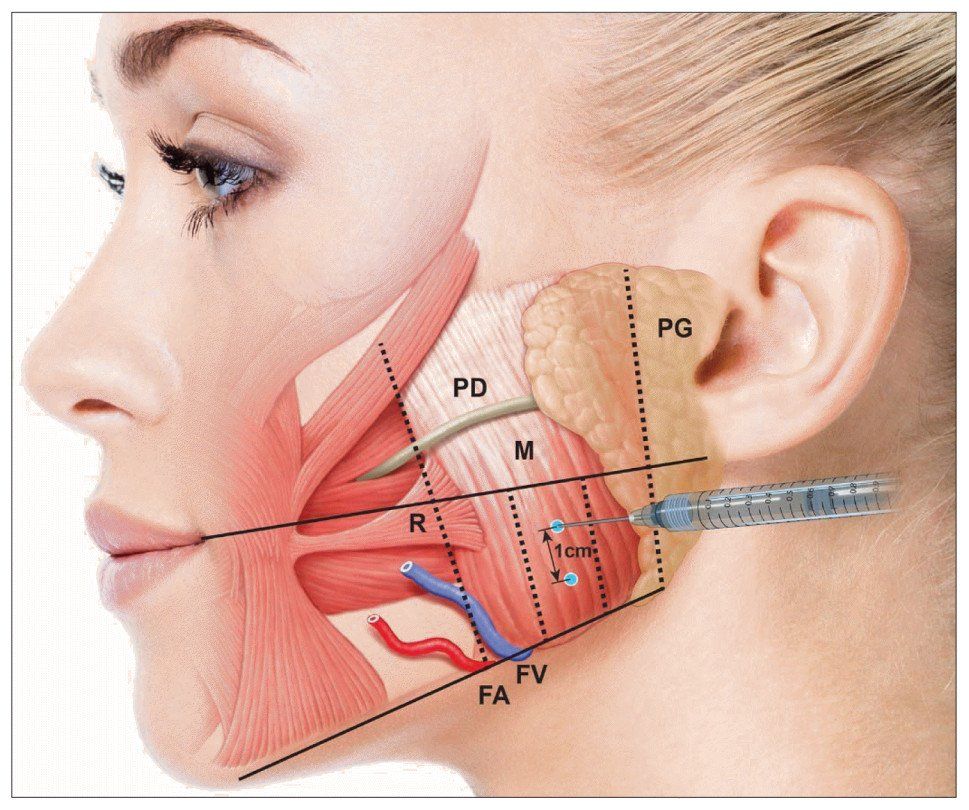
The TMJ allows you to speak, chew, yawn and swallow. It functions through a precise system of muscles, ligaments and an articular disc that absorbs the enormous pressures generated during chewing and prevents friction between the bones.
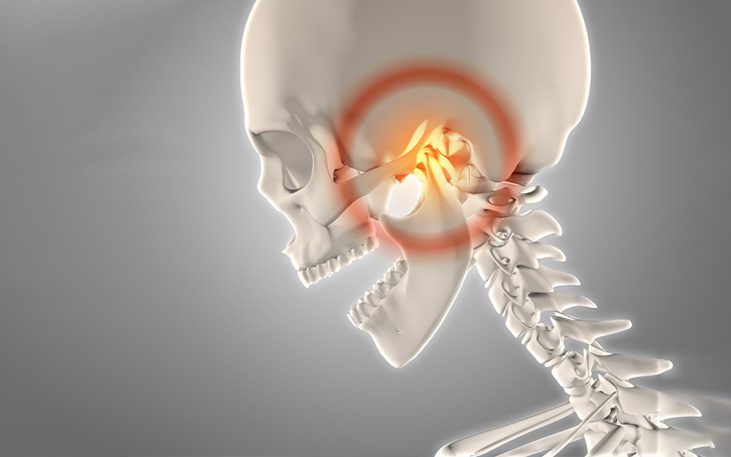
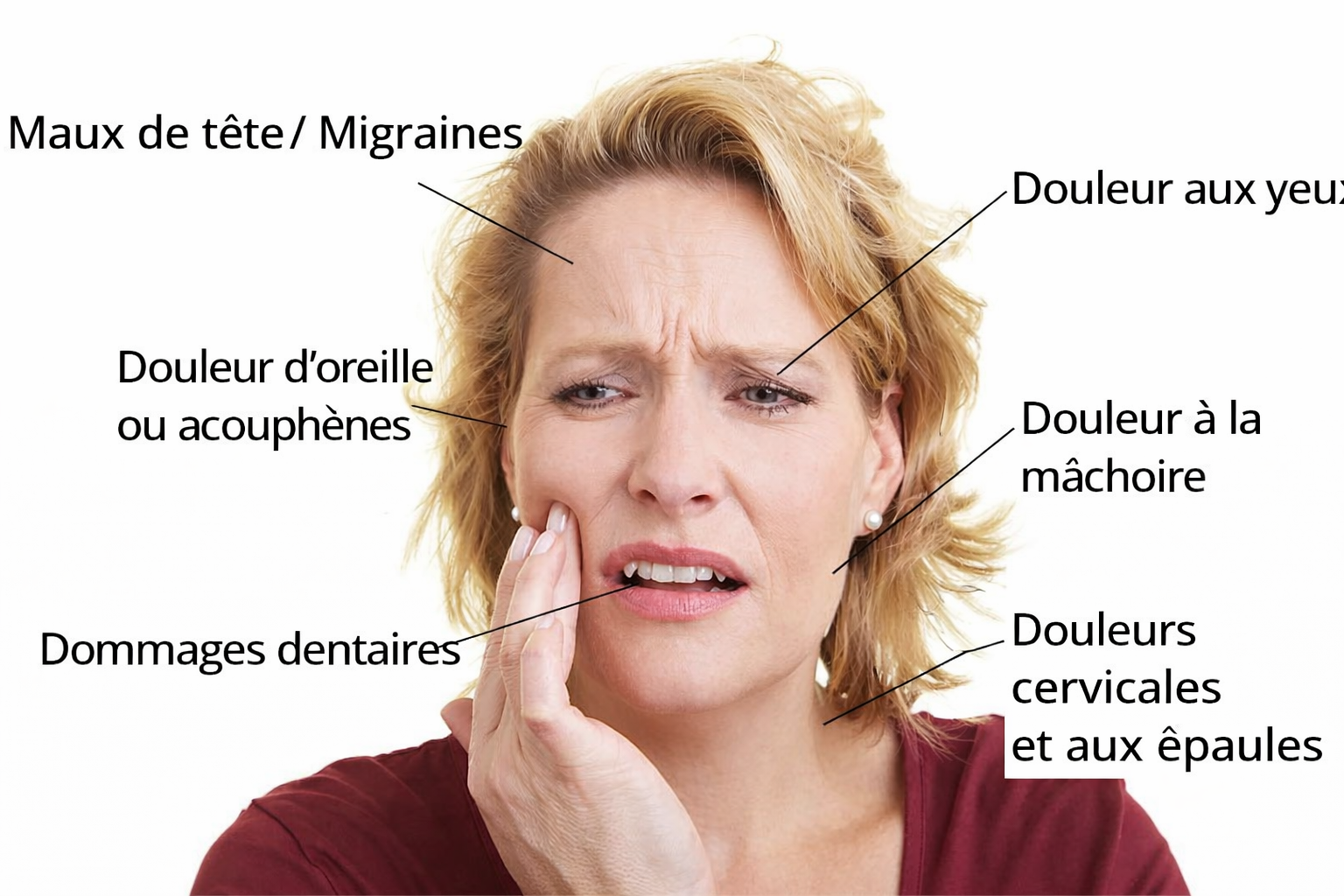
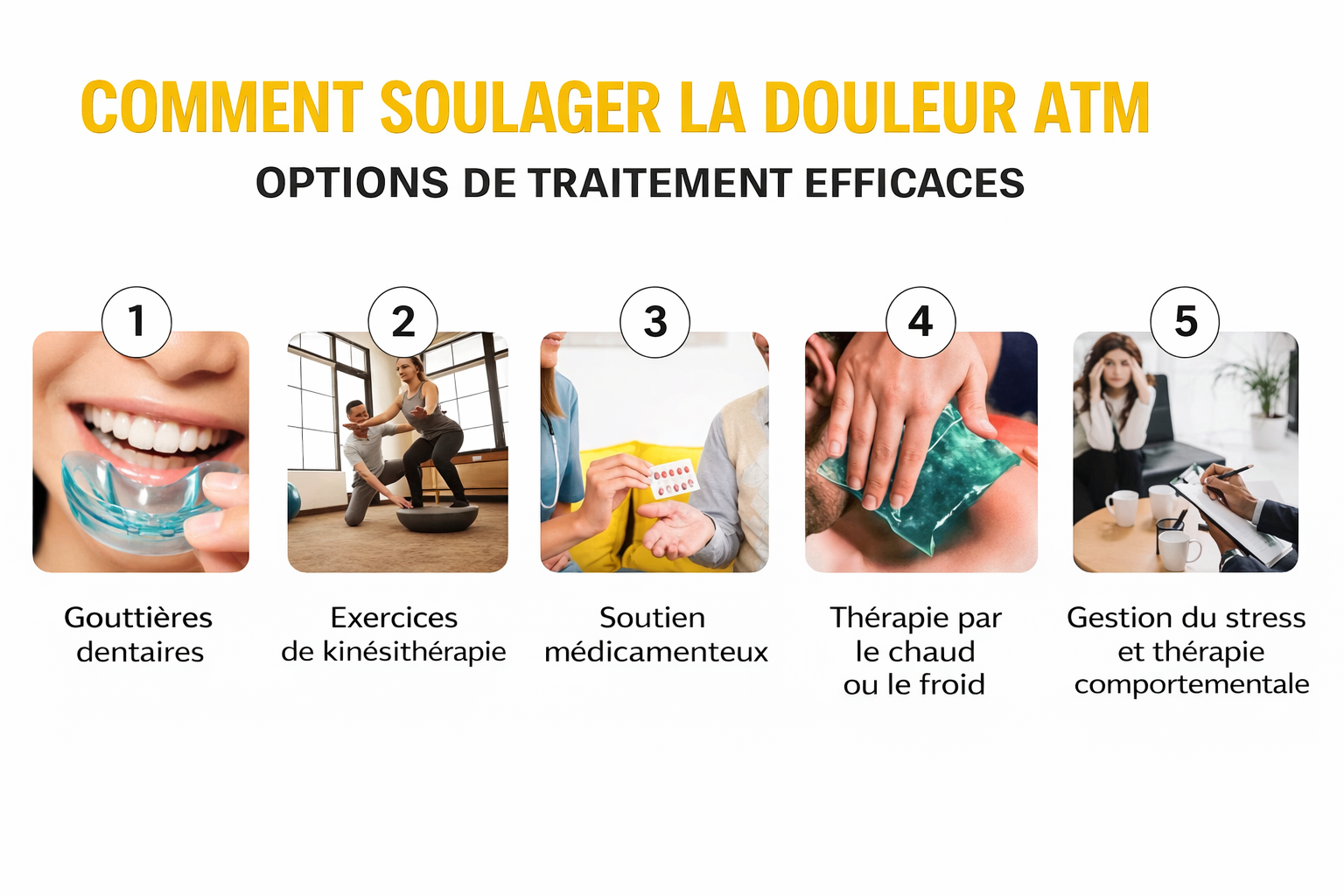
TMJ disorders (also called temporomandibular disorders or TMD) occur when this joint or the muscles surrounding it do not function properly, causing pain, limited movement and various symptoms that can severely affect your quality of life.